Answer 3
The problem:
In spite of taking optimal medications for hepatic decompensation, the patient who was compensated before surgery complains of symptoms which are strongly suggestive of hepatic decompensation, so is this the only possibility or there may be other subtle problems?
@ Letters from internal
medicine residents:
-An Email from dr.Ali Abou-Taleb: "...This is a case of a decompensated
liver disease besides hypothyroidism which resulted from thyroidectomy
done recently."
(Hoping for more of your valuable answers, Thank you Ali)
-Another Email from Ahmed Hamdi :
"....in the 1st place I think all these symptoms can be explained by the
patient's liver chronic disease as I'm impressed from the patient's
social and clinical background as in this scenario: he had previously a
known chronic liver disease with only recent exacerbation and this
diagnosis is supported objectively by ascites, increased enzymes levels,
hepatosplenomegaly, +ve HCV and bilharzial markers, edema, megaloplastic
anemia (may occur in liver disease due to Vit B stores depletion), as
symptoms are non-specific and frequent in these cases and without
objective neurological findings for the lower limbs weakness. So the
cause of this patient's liver disease is probably chronic hepatitis and
portal hypertension .
Hypothyroidism after op. is suggested but without information about the
gland function condition before the op. and I suggest that it is a
coincidence with the liver disease.
There is another scenario that occurred to me ........ :
Occurrence of all these multiple organ affection:
-hepatitis with hepatic function decompensation
-? goiter with hyper- or hypo-thyroidism causing thyroidectomy
-Vit B12 deficiency due to pernicious anemia causing megaloblastic
anemia
-proximal muscle affection with weakness and cramps
-unspecific general symptoms: asthenia, easy fatigue and generalized
heaviness
may be explained by some sort of autoimmune disease causing: hepatitis,
thyroiditis, myositis and pernicious anemia and so explained all the
symptoms of the patient.
As I mentioned the patient's social and clinical background (a farmer,
bilharziasis and high chance of HCV infection) besides the
epidemiological high prevalence of such cases in the patients pool we
encounter every day working, so I think it would be tricky to us:
inexperienced and not deeply-thinking young practitioners. Again looking
at the big picture is the clue I think."
(A lengthy letter but you and Ali agreed about his opinion)
To Elucidate The
truth:
Really I agreed about the second half of your answers as the primary
problem especially in this patient and in even many patients who we
simply accept as having liver disease decompensation but without looking
in a logic manner at the special circumferences of the case.
This is a case of hypothyroidism in this scenario:
A compensated liver-diseased patient who had thyroidectomy
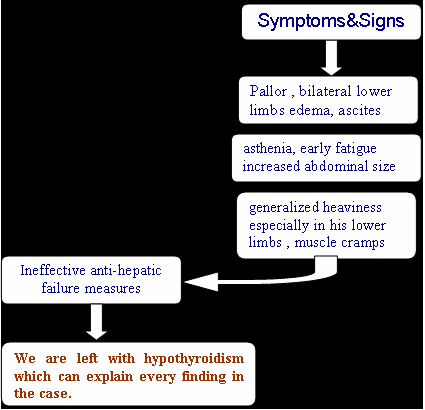
Treatment of course is thyroxine replacement.

