Case 5
A diagnosis
not to miss
This case was
emailed to me by Dr.Magdi
Nagiub to be consulted about.
Personal history:
Male patient 23 years old married for 4 months
(Driver), smoker about 20cigarette/day for 5 years with occasionally
Hashish intake.
Complaint:
Easy fatigability of 2 weeks duration, gradual onset and progressive
course.
History
of the present illness:
-Not diabetic or hypertensive.
-The condition started 2 weeks ago by headache, blurring of vision,
exertional dyspnea, muscle cramps and bilateral loin pain, he sought
medical advice but without improvement.
-Four days ago he developed abnormal movement in the eye lids, face,
upper and lower limbs (??Tics) that were observed by others.
-Then developed generalized tonic clonic convulsions followed by tongue
biting loss of consciousness and frank haematuria, then he was brought
to us for our medical attention.
-At our department he developed another attack of fits.
-Three days after admission developed disturbed conscious level, left
sided weakness and right gaze deviation of the eyes (?? stroke).
Examination:
Pulse:80 BP:120/80
Moderate pallor, Tinge of jaundice
Mild hepato-splenomegaly.
LAB:
CBC: Pancytopenia
Reticulocytic count: 17.6 corrected retics: 6.6
Total bilirubin:1.4 direct bilirubin: 0.3
Normal liver and renal function
Urine analysis: Normal
Recent CT brain : Normal
And I knew today that the patient has died in
the ICU.
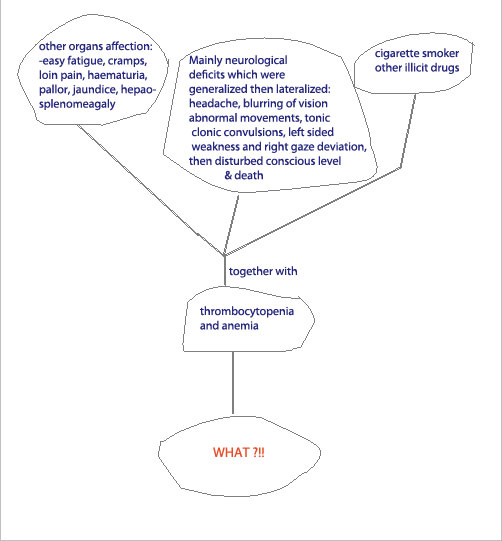
To summarize things up:
So to explain the multisystem affection,
especially CNS with normal CT, I'd like to begin from the prominent
ischemic vascular injury caused by microvascular disease.
So what caused this?
Thrombocytopenia,
anemia (caused by microvascular hemolysis) elucidate the cause as to be a
case of TTP (thrombotic thrombocytopenic purpura).(revise the literature
below.)
The treatment of choice here is plasma
exchange.
So if this young patient were to be diagnosed
early and correctly right action could have been taken.
THROMBOTIC MICROANGIOPATHIES
|
|
1. |
Epidemiology.
The thrombotic microangiopathies are characterized by
excessive platelet aggregation, which leads to microvascular
occlusion, thrombocytopenia, and mechanical injury to
erythrocytes (microangiopathic hemolytic anemia).
|
|
a. |
Platelet
aggregation primarily within the systemic
microvasculature causes TTP, whereas that affecting
predominantly the renal circulation is known as
hemolytic-uremic syndrome (HUS). Clinical
distinction between the two entities is not always
straightforward, and they are often described as a
single disorder. However, studies demonstrate
distinct histopathologic findings in the two disease
states, suggesting different underlying
pathophysiologies. |
|
|
b. |
Thrombotic
microangiopathy has also been described in
association with certain drugs (e.g., ticlopidine,
mitomycin), after allogenic bone marrow
transplantation, during pregnancy, and postpartum.
|
|
|
|
2. |
Pathophysiology.
|
|
a. |
The
microvascular thrombi that characterize TTP and HUS
consist of platelet aggregates with abundant von
Willebrand factor (vWF). Endothelial cells and
megakaryocytes produce multimers of vWF that bind to
platelet glycoprotein Ib receptors. ADAMTS 13 is a
vWF-cleaving metalloprotease present in plasma. In
TTP plasma, ADAMTS 13 activity is less than 5% of
normal. As a result, the large multimers of vWF are
not cleaved; instead, they remain anchored to the
endothelium, allowing passing platelets to adhere
and form potentially occlusive platelet thrombi.
|
|
|
b. |
In
contrast, plasma ADAMTS 13 activity is largely
normal in HUS. Shiga toxin–producing Escherichia
coli (E. coli 0157) is believed to be the
predominant etiological agent of HUS in children and
occasionally causes HUS in adults. Shiga toxin
enters the circulation and attaches to the
glomerular capillary endothelial cells, where it
induces the endothelial cells to secrete large
multimers of vWF, causing platelet activation and
microthrombus formation.
|
|
|
|
3. |
Presentation.
|
|
a. |
More than
90% of patients exhibit the classic pentad of signs
and symptoms characteristic of TTP:
thrombocytopenia, microangiopathic hemolytic anemia,
neurologic abnormalities, renal abnormalities, and
fever. |
|
|
b. |
In
practice, however, the triad of thrombocytopenia,
schistocytosis, and elevated lactate dehydrogenase
should raise the physician's suspicion of TTP,
particularly in the absence of an alternative
explanation for these abnormalities.
|
|
|
c. |
The extent
of microvascular aggregation is reflected in the
degree of thrombocytopenia, erythrocyte
fragmentation (schistocytes, helmet cells), and
elevation of lactate dehydrogenase.
|
|
|
|
4. |
Diagnosis.
The availability of effective treatment for TTP makes early
diagnosis essential. This urgency has led to decreased
stringency in the five diagnostic criteria as they were
originally described in 1966.
|
|
|
5. |
Management.
|
|
a. |
A single
randomized clinical trial demonstrating the
superiority of plasma exchange over plasma infusion provides the only
firm evidence on which to base recommendations for
treatment in TTP.
|
|
|
b. |
Plasma
exchange is the combination of plasmapheresis (which
may remove unusually large multimers of vWF and
autoantibodies against ADAMTS 13) and infusion of
fresh frozen plasma or cryosupernatant (containing
additional metalloprotease). It is the primary
treatment of adults with acquired acute idiopathic
TTP and should be initiated as early as possible in
the course of the disease. Its increased
availability over the past 20 years has dramatically
improved survival rates in this disease from 10% to
approximately 90%. Initially, plasma exchange should
be performed once daily. The value of additional
treatment modalities (including glucocorticoids) is
unknown.
|
|
|
c. |
In the
absence of life-threatening hemorrhage or
intracranial bleeding, platelet transfusions
should be avoided because they can exacerbate
microvascular thrombosis.
|
|
|
d. |
The role of
plasma exchange in adults with HUS is much less
clear, and it is generally felt to be ineffective in
this patient group.
|
|
Submit your comment through the
following section